
Occupational licensing is when the government requires people to complete educational and training programs, pass tests and pay fees in order to do a job legally. State officials, often in unelected administrative or bureaucratic roles, typically determine the requirements. Occupational licenses are meant to protect the public from people unfit to provide certain services. In Michigan, approximately 180 occupations are licensed by the state.
But research finds little evidence that occupational licensing laws improve the quality of services or public health and safety. Experts and economists across the political spectrum, including the labor departments of the Obama, Trump and Biden administrations, recognize the need for reform. This report explains the positive reforms lawmakers in Michigan have done, but also identifies more ways to improve these laws and help Michiganders get to work.
Occupational licensing is when the government requires people to complete educational and training programs, pass tests and pay fees in order to do a job legally. State officials, often in unelected administrative or bureaucratic roles, typically determine the requirements. Occupational licenses are meant to protect the public from people unfit to provide certain services.
Proponents of licensing believe that requiring people to get state approval before they can work guarantees a minimum level of quality. But lawmakers and licensing agencies rarely consider how well occupational licensure laws deliver on this goal.
And there are costs. In Michigan, approximately 180 occupations are licensed by the state. This has negative effects for people trying to find jobs and for consumers. State licensing requirements restrict who can practice a trade, which means fewer people will work in those fields. This artificially decreases supply, reduces competition and increases costs to consumers.
Licensing laws tend to become entrenched. Workers who are already licensed adamantly defend them, because they benefit directly when the state restricts who can compete in their industry. The harms related to licensing, meanwhile, are felt only minimally by individual consumers. They are well hidden among all the other factors that contribute to rising prices, such as inflation, tax burdens and energy rates.
Experts and economists across the political spectrum, including the labor departments of the Obama, Trump and Biden administrations, recognize the need for reform. Both the left-leaning Brookings Institution and the libertarian-leaning Mercatus Center agree that these mandates are often arbitrary, do little to enhance consumer safety and primarily benefit special interest groups. Most licensing laws restrict people with a criminal background from obtaining a license, and research suggests these laws contribute to higher crime rates, as ex-offenders have fewer employment options.
Research finds little evidence that occupational licensing laws improve the quality of services or public health and safety.[1] They raise wages for licensed workers, but this comes at the expense of higher prices for consumers and more unemployment in the economy.[2] The evidence suggests that licensing laws persist primarily because existing firms advocate for them to restrict their competition and boost their income and profit. Licensing requirements also present a barrier to people moving from state to state.[3]
The most comprehensive study on the economic effects of licensing at the national and state level finds that it costs the economy more than 1.7 million jobs and up to $184 billion annually in potential economic output. The estimated impact in Michigan is a loss of 80,000 jobs and an annual cost of nearly $8 billion in misallocated resources.[4]
Licensing laws do not appear to produce higher quality services. Even if they did, the value of the improved quality must outweigh the costs imposed by these laws. A study published by the National Bureau of Economic Research in 2020 found that there was no relationship between how stringent a state’s licensing laws are and the ratings consumers give service providers. The study did find, however, that more restrictive licensing laws are associated with less competition and higher consumer prices.[5]
A more recent study examined consumer reviews of different businesses on the borders of states with significantly different licensing laws. If these laws improved services, consumers should rate them noticeably higher in states with strict licensing requirements compared to consumers in neighboring states with lax or no licensing mandate. The researchers found no connection between licensing requirements and consumer reviews in most occupations they examined. The only statistically meaningful differences identified suggest that less burdensome licensing is associated with higher service quality.[6]
The negative impact of licensing laws is probably most firmly felt in industries that pay relatively low wages but are highly regulated. Research from the Institute for Justice, for example, finds that licensing rules for cosmetologists lead aspiring workers to fail to graduate on time, accumulate more college debt and default on loans. Michigan law requires cosmetologists to complete 1,500 hours of education and training. This costs on average more than $16,000 per year.[7]
Another measure of the value of licensing laws is how well they stand up when scrutinized by the government. Several states conduct “sunrise reviews” of their licensing laws, which are formal reevaluations of the need for mandating a license. An analysis of nearly 500 of these reviews from different states found that licenses are not recommended 80% of the time.[8] Michigan does not have a statutorily required sunrise review process.
Only a small number of studies examine the effect occupational licensing has on public health or safety. The limited evidence suggests that these state-imposed mandates do little to protect the public.
A study from the Obama administration reported:
“Stricter licensing was associated with quality improvements in only 2 out of the 12 studies reviewed. There is also evidence that many licensing boards are not diligent in monitoring licensed practitioners, which contributes to a lack of quality improvement under licensing.”[9]
If licensing fails to show clear benefits in the quality of services provided, it is unlikely to provide meaningful health and safety benefits.
Positive health and safety effects should be easy to find in dangerous occupations or the health care industry. Existing research generally fails to find a correlation between licensing and improved outcomes in these areas, however. In some cases, the research suggests the opposite: that licensing laws negatively affect health-related outcomes.
Electricians work in a relatively dangerous profession, with a much higher death and injury rate than the average occupation.[10] A study from the Bureau of Labor Statistics examined the licensing of electricians from 1992 to 2007. It focused on states that began licensing electricians over this period, analyzed the strictness of these regulations and compared worker injury and death rates across states. The report showed that “the impact of occupational regulation on deaths and injuries is statistically insignificant or indeterminate.”[11]
The bulk of studies looking at the licensing requirements of nurses suggest that these rules harm, rather than help, the public. One example is nurse practitioners, who are nurses with advanced medical degrees and extra training. Licensing and scope of practice rules vary among the states, with 22 permitting nurse practitioners to operate independently. Other states, including Michigan, restrict these medical professionals from providing certain services and require them to operate under the direct supervision of a physician.[12] The graphic below shows the various types of scope of practice laws across the country. It was created by the School of Nursing at Simmons University and based on information provided by the American Association of Nurse Practitioners.
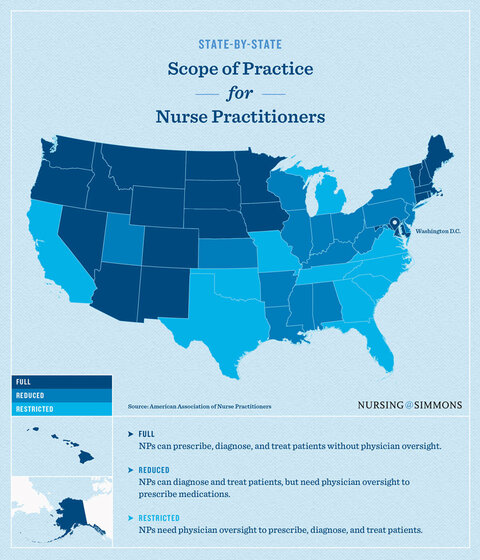
Research shows restrictions on the scope of practice of nurse practitioners is associated with lower wages, an increased likelihood of nurses relocating and worse health outcomes for some populations. One study found that health insurers had to pay between 3% and 16% more for well-child visits in states with restrictive licensing laws for nurse practitioners. It also found “no evidence that the changes in regulatory policy are reflected in outcomes that might be connected to the quality and safety of health services.”[13] Another study found nurse practitioners were far more likely to move to full practice states than restricted practice states.[14] A 2022 study found that parents rated their children’s health better in states that allow nurse practitioners to practice independently.[15]
More than 750,000 people in Michigan have active licenses that are overseen by the Bureau of Professional Licensing.[16] This represents 17% of the 4.4 million nonfarm jobs in the state.[17] And while this department oversees more than 40 of the state's occupational licenses, there are dozens more that fall under the control of other state agencies and boards. This includes more than 100,000 public school teachers and thousands of other school employees, some of whom need licenses or certifications.[18] Altogether, including some licenses required of businesses, Michigan requires licenses, certification or registration for more than 400 different occupations or industries.[19]
Michigan is in the middle of the pack nationally for the number and strictness of its licenses. A report published by the Archbridge Institute ranked states by these measures and pegged Michigan at 29th worst among the 50 states.[20] The Great Lake State fell in the middle among its neighbors too, with Wisconsin and Ohio having higher licensing burdens and Illinois and Indiana having less restrictive ones.
For lower-income or working-class occupations, Michigan requires fewer licenses than the national average, and the state generally has smaller fees and less mandatory training.[21] But the Michigan Constitution stands apart, according to the Mercatus Center, because it requires the boards that oversee and create licensing requirements to be controlled by people who are already licensed in the profession.[22] This may provide an incentive for licensing boards to restrict access to an occupation, harming competition.
Michigan requires a state license for about 180 different occupations, and its licensing agency receives $540 million annually to regulate these occupations.[23] This revenue comes from state tax revenue as well as from fees paid by license holders.

A common assumption is that the workers and businesses regulated by governments oppose such rules. When it comes to occupational licensing mandates, however, the regulated industries and occupations are typically supportive of the regulations. People already working in licensed occupations benefit when the state forces their would-be competitors to get a license before operating legally. The mandates limit competition and reduce the supply of labor, increasing the price for the services provided by those who are licensed.
If more people understood this dynamic, lawmakers might be less supportive of occupational licensing. Efforts to scale back these laws, however, suffer from a dynamic that economists call “concentrated benefits and diffuse costs.”[24] This theory explains situations where laws that cause more harm than good remain in place, even in a democratically controlled government. The reason is that these laws benefit a small special interest group — people who get the concentrated benefits — and this group will go to great lengths to protect those regulations and the benefits they provide. The harms, on the other hand, are diffuse. They do not impact the typical taxpayer or consumer in a significant way. In other words, the regulated industry faces strong incentives to preserve its benefit, while the average voter has little or no incentive to push for change. As a result, reforming licensing laws remains of little importance for most voters.
This is related to a theory developed by economist George Stigler, which he called “acquired regulation.” He wrote, “We propose the general hypothesis: every industry or occupation that has enough political power to utilize the state will seek to control entry.”[25] Today, this is more commonly referred to as regulatory capture.
This occurs when an industry or occupation uses the power of government to benefit itself. People in these industries advocate for state lawmakers to create regulations, such as licensing requirements. These laws can be designed in such a way as to provide a competitive advantage to existing firms. For instance, proposed licensing requirements often contain “grandfather clauses” that grant licenses automatically to people already employed in the occupation. Incumbent firms also benefit when state-imposed regulations make compliance relatively more expensive for new firms seeking to enter the market.
There are many examples in Michigan showing that regulatory capture is common and that regulated industries work to protect their concentrated benefits by opposing reforms. In just the past few years, industry groups and occupational associations have proposed new licenses and regulations and successfully thwarted the loosening of some existing licensing requirements. In each case, the regulated industry clearly benefited at the expense of consumers and would-be competitors. Below are several examples.

Aspiring barbers need 1,800 hours of training in Michigan. Legislation was introduced in 2012 that would repeal this requirement along with a mandate that barbers attend an in-person college. Michigan Barber School Director Darryl Green said he was “in shock” that lawmakers were considering eliminating these requirements. He explained: “It does have a lot to do with public health. I’m not saying we are as important as doctors, but we are the closest you can get. We are turning this into the Wild, Wild West. … I’d like to see them get a haircut in a barber shop five years from now. It will be like rolling the dice.”[26]
Raising the specter of an industry turning into the Wild West is a common refrain from groups benefiting from the limited competition and higher prices licensing requirements produce. It’s mostly a red herring, though. Nothing would prohibit barbers from logging 1,800 hours of training if they thought it was useful and gave them an advantage over their competitors. That few would do this training if it were not required suggests that it is not providing much value. The more likely reason the director of the Michigan Barber School is opposed to eliminating required training mandates is that his employer would lose the business of providing this training to would-be barbers.

In 2019, 2020 and again in 2023, Michigan lawmakers proposed licensing requirements on hunting and fishing guides. These new rules would mandate fees, CPR training, annual reporting and prevent anyone with a criminal record from the field. One of the sponsors of these bills noted that current hunting and fishing guides are driving the effort and said, “This is a package of bills that has been one of the main goals for many of our hunting and fishing organizations in this state for the last several years.”[27]

Michigan repealed its licensing law for dietitians and nutritionists in 2014 after a state review committee found “lack of clear public health and safety benefits.”[28] But in 2021, a bill to reestablish these licenses was proposed. It would require dietitians and nutritionists to obtain a college degree (nutritionists would need at least a master’s degree), complete 1,000 hours of supervised practice, pass exams, pay fees and take continuing education courses.[29]
People currently operating in these fields — many of whom would be automatically granted a license — supported the imposition of these requirements on others. Ann Hoffman of the Michigan Academy of Nutrition and Dietetics said: “Licensure ensures the most qualified, educated and well-trained professionals will treat chronic illness and disease. There are no alternatives to state regulation of the occupation that adequately protect the public from risk of harm which is real in Michigan.”[30]

In 2020, the Legislature approved more regulations on funeral home directors. The new law required people working in these fields to pass state and national exams and accumulate continuing education hours to maintain a license.[31] It also makes it harder for individuals from other states to get licensed in Michigan. As noted in media reports, the representative who introduced the bill is a funeral home operator. Interest groups representing funeral homes and schools offering mortuary science courses supported the bill.[32] It was signed into law in December 2020.
Those groups will be the chief beneficiaries of these more stringent requirements. They will result in more revenue for schools offering mortuary science courses and less competition for existing funeral homes. Individuals and businesses with a license already would be grandfathered in, so most of these new requirements will not apply to them, only to their future competition.

A Michigan law requires property managers working for someone else to have a real estate license. An attempt to repeal this requirement was defeated, with the Michigan Realtors Association, a group representing licensed realtors, leading the opposition. Restricting property management services to license holders reduces supply and limits competition for realtors.[33]

Associations representing musical therapists supported a new licensing requirement for the occupation in 2019. The bill would have mandated a college degree, 1,200 hours of clinical training, a board exam and hundreds of dollars in fees and testing costs.[34] It stalled in committee and was not made into law.

Michigan statute requires fire sprinkler installers to have a contractor’s license. A 2019 proposed law supported by fire protection associations would have made the mandates much more stringent. The bill, which did not pass, would have required a four-year apprenticeship, 8,000 hours of practical experience, 280 hours of classroom time and hundreds of dollars in annual fees.[35]

Food delivery drivers would have had to obtain a certificate to practice in Michigan if a 2022 bill had passed. They would have to pass a test and possibly receive training as well. The sponsor of the bill owns a chain of restaurants that primarily offer dine-in services.[36]

A requirement that solar panel installers obtain an electrician license was introduced in the Michigan Legislature in 2021. The bill passed the House but stalled in the Senate. It had broad support from special interest groups representing licensed electricians.[37]

Naturopathy is treating patients with natural remedies, such as vitamins, herbs and organic food, as well as coaching clients in self-healing, such as exercise and lifestyle change. State and national groups representing currently practicing naturopathic physicians advocated in 2018 to establish a state license for this practice, which would have required a college degree, fees and testing.[38] The bill passed one chamber of the Legislature but did not progress further.[39]

The Michigan affiliate of the American College of Nurse-Midwives developed a bill to require professional midwives to obtain a state license to practice. The Legislature approved and it was signed into law in 2017.[40] The licensing requirements mandate that midwives pay a $650 upfront fee, a $400 renewal fee, complete an accredited training program, obtain 30 hours of continuing education and more.[41]

Lawmakers have repeatedly tried to loosen the occupational restrictions on nurses in Michigan, only to be stymied by groups benefiting from the current laws. In 2020, for example, a bill passed the Legislature that would have had Michigan join 38 states in a nursing compact. The compact would make it easier for hospitals to hire nurses with experience in other states. It was opposed by the Michigan Nurse Association Board and some unions and ultimately vetoed by Gov. Gretchen Whitmer.[42]
Michigan has some of the most restrictive rules on nurse practitioners in the county.[43] While other states let highly trained nurses write prescriptions and run their own medical clinics, Michigan law severely limits their practice. When lawmakers tried to loosen these rules and allow nurse practitioners to work independently, the state medical associations — comprised mostly of physicians who benefit from these restrictions on nurses — came out in opposition.
Rose Ramirez, a physician and former president of the Michigan State Medical Society, said this about the effort: “The best health care teams are physician led. I worry about the safety of the patients in our state who deserve to have well trained physicians supervising their care.”[44] These rules were relaxed during the COVID-19 pandemic. But Gov. Whitmer then reinstated them, against the advice of her health advisor.[45]
Occupational licensing laws harm people in subtle ways that are often difficult to detect. Millions of consumers spend slightly more on services because supply and competition are artificially limited. Thousands of workers persist in less preferred jobs because they cannot afford the requirements to get licensed to work in the field of their choice. But there are also those who are directly harmed by state licensing laws. Here are some examples.

Ntcharba Chabi is a hair braider trying to earn a living by running Blanca’s Braids in Garden City. After a competitor complained that Chabi was not properly licensed, she received a cease-and-desist order from the state and was fined. State regulators said she needed a cosmetology license even though this license is not required to braid hair. The problem was Chabi’s salon possessed a shampoo bowl and only licensed cosmetologists can charge customers for shampooing hair. Getting the license requires 1,500 hours of training, hundreds of dollars in fees and a test.[46]

Austin Loose owes thousands of dollars for schooling and testing for training he will likely never use. While other states allow massage therapists to work without government-mandated training, Michigan requires 500 hours and passing a test. Austin and his twin brother Login went to school to learn massage therapy and graduated together. Austin’s learning disability, however, interfered with his ability to pass the final test. While Login got his license, Austin is stuck working lower-paid jobs.[47]

Dr. Jan Pol is a veterinarian in rural Michigan who once starred in a reality TV show aired by National Geographic. An out-of-state vet reported him to the state for not wearing the proper surgical attire and failing to provide a warming pad for a dog. This stemmed from an incident where Pol saved a dog’s life after it was hit by a car. The dog’s owner made no complaints about the service Pol provided. Still, the state licensing department alleged negligence and incompetence under state law and slapped Pol with a fine and probation.[48]

Mike Grennan is a carpenter and Laurence Reuben a nurse. But their past criminal mistakes restrict them from getting a license in their fields. Grennan can work for other construction companies or on jobs billed for less than a set amount of money, but he cannot work for himself. Reuben has a low-level felony conviction from New York state, but he went through a rehabilitation program and was legally working as a licensed nurse there. When he moved to Michigan, however, the state denied him a license because of his criminal record.[49]

Donna Williams is a Michigan native who spent $25,000 and got nearly 500 hours of training in California to do makeup artistry. She has worked on film and video projects in Michigan, but her license doesn’t transfer or allow her to work as an esthetician or cosmetologist. “I’m going to be 67, I’m on a fixed income. I absolutely love Michigan, but you just can’t make enough money this way,” she said. Williams moved away from her home all the way to Las Vegas to find less regulated makeup jobs. “I was born and raised in Michigan,” she added. “Of course, I want to stay and use my talents in my home state, but my home state makes that almost impossible.”[50]
Stephanie Brown owns a highly rated salon in Kalamazoo that specializes in hair braiding. A nearby competitor complained to the state that one of her employees was washing clients’ hair but did not have a license to practice cosmetology. “All it takes is someone who doesn’t like you and then there goes your business,” Brown said. The employee has since left, but Brown is still stuck paying the fines. The typical salon worker makes an annual salary around $30,000 per year but is required to take training that involves 25 times the hours that residential home builders must take.[51]
Shaketra Payne is a certified natural hair culturist who braids hair. Many people need their hair to be recently washed to be properly braided. In order to wash hair in a salon, something done every day by people in their own homes, Michigan law mandates that a person have a cosmetology license that requires 1,500 hours of training. Payne had to turn away an elderly woman in a wheelchair because her hair was not clean enough to do dreadlocks. Lacking a cosmetology license, she could not legally wash this woman’s hair in her salon. “It just broke everybody's heart that she literally looked like she wanted to cry,” Payne said. “I'm not a cosmetologist, and I don't want to be a cosmetologist. I want to be a hair braider.” She added, “[I]t was just like a slap in the face that I can't even wash my own clients' hair.”[52]
People who do very similar work are regulated very differently in Michigan. This suggests that occupational licensing rules are established for reasons other than considering what constitutes a risk to public health and safety. If this were the primary concern, similar occupations would have similar regulations. These disparities highlight why occupational laws need to be regularly reviewed to ensure they are consistent and necessary.
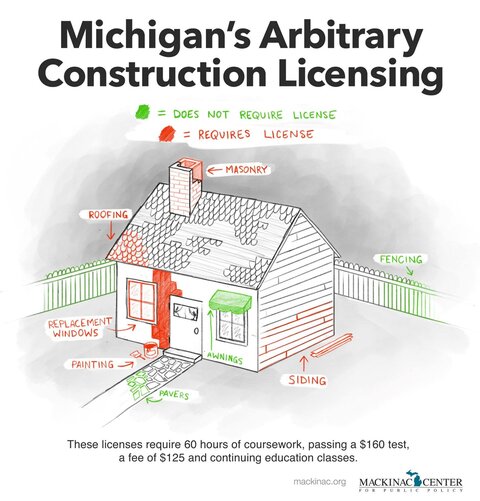
In Michigan, for example, one needs a license to lay wood or tile floors but not to install vinyl or carpet flooring. You need a license to construct a concrete driveway but not one made of asphalt. Roofing a house requires a license but not erecting awnings under the roof. You need a license to knock down a house, but not to pick it up and move it. Carpenters and insulators need to fulfill licensing requirements but not people who only build fences or install plaster walls. Adding siding to the outside of a house requires a license but not putting up the drywall on the inside of the house.[53]

There is also a blanket exception to the license mandate for construction-related work that costs less than $600 or is performed by a volunteer.[54] If licensing requirements were strictly necessary to maintain safe working conditions, there would be no rationale for allowing exemptions.
But there’s an even broader exemption to licensing requirements: volunteer labor. This is nicely exemplified by the goodwill of a Michigan school superintendent. To avoid hiring a licensed company to repaint the district’s school buildings and save $150,000, Superintendent David Harnish spent his summer in 2018, alongside some of the district’s students, painting the buildings himself. At the time, state law required painters to be licensed and spend 60 hours in training and pass a test. But because Harnish and these students were volunteering their labor, the licensing law did not apply. The Michigan Legislature repealed licensing requirements for painters later that year.[55]
Librarians who work in Michigan public schools need a bachelor’s degree, a teacher certificate and a library media endorsement. These are stricter requirements than those in surrounding states, and the head librarians at small community libraries can work legally after earning only a high school diploma or GED.[56]
Selling produce like apples, tomatoes, corn, lettuce and cabbage requires no state license. Sales of honey, maple syrup, apple cider and eggs are only regulated if your annual sales exceed certain levels. But selling meat, fish, mushrooms, garlic, herbs, bagels, doughnuts and cookies are strictly forbidden without first obtaining a state license.[57]
A nursery grower license is needed to grow and sell some plants. This includes “trees, shrubs, perennials, mums, fruit trees, berry plants, rose bushes, vines, herbs, and bulbs that are capable of surviving the winter, without special care.” It does not include “annual plants, cut flowers, Christmas trees and greens [or] cut herbs.” The state of Michigan also does not regulate those growing and selling fruit, vegetables or wild trees, shrubs, vines or flowers from roadside stands.[58]
The amount of training required by Michigan’s licensing laws often appears arbitrary or disproportionate in many cases. Below are some examples.
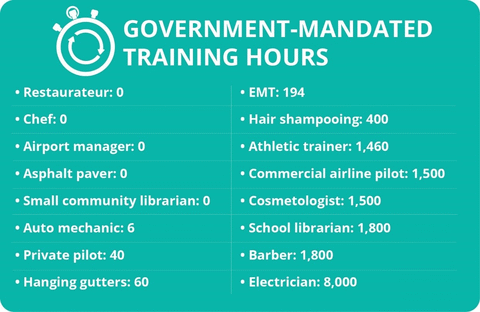
Michigan passed a series of licensing reforms over the past decade. The state repealed eight license or registration requirements outright. This included auctioneers, community planners, dieticians and nutritionists, immigration clerical assistants, interior designers, ocularists, painters and school solicitors.[63]
The state also reduced regulatory requirements in other areas, such as allowing mobile cosmetology services, increasing the scope of practice of clinical counselors and nurse anesthetists, eliminating the continuing education hours for athletic trainers, allowing barbers to meet their licensing hours through an apprenticeship and recognizing the licenses of dental therapists earned from other states.[64]
In 2018, the Michigan Legislature prevented local municipalities from mandating their own occupational licenses. Specifically, no city, township, village or county or their public authorities in Michigan can require any training, education or fee as a condition of performing work in any specific occupation. If the license was in place before 2018, it could continue, but it is overridden by any licensing requirements from the state.[65]
Bay City requires a license for fortune-tellers.[66] Lansing has one for auctioneers.[67] Grand Rapids mandates people obtain permission from the city and pay $421 before they can snowplow.[68] The city of Detroit required occupational licenses for landscapers, window washers, movers and dozens of other jobs.[69] The city began repealing many of these after the 2018 state law went into effect.[70]
Michigan lawmakers in 2020 revised laws that required people to have “good moral character” to obtain a state license. This provision was commonly used to prevent people with a criminal record from getting licensed. The reforms reined in the use of this requirement in several ways. They limited regulators to including someone’s criminal record in licensing decisions only if it contained multiple civil actions or a felony conviction. The felony must have a “direct and specific relationship” to the job the person would do if licensed and be a “demonstrable risk” to public safety. Denying someone a license based on a past felony conviction now requires regulators to contend that the applicant would be more likely to commit a crime with the license than without it.[71]
This law immediately made it easier for former prisoners to find work. One construction worker was finally able to open up his own business and make a living.[72]
These reforms have limitations, however. In many occupations, especially in the health and government industries, restrictions on people with criminal records are written directly into the individual statutes that apply to this employment. That is, prohibiting people from working is not based on the “good moral character” provision in the licensing laws, so the 2020 reforms did not apply in these cases. The reforms also specifically do not apply to child care and nursing home workers or police officers.
The bill package also requires the state licensing agency to report annually how many people it denied licenses to because of a lack of good moral character.[*]
In the two years since the law went into effect, licensing regulators approved more than 9,500 new licenses and denied zero for lack of good moral character.[73]
Lawmakers in 2021 made it easier for active military members, veterans and their families to find work in Michigan. New laws waive licensing or registration fees and recognize any occupational license earned from another state for military families. More than one-third of military spouses work in a field requiring a state license, and this group is more likely to be unemployed compared to the general population. These reforms make it easier for them to find a job and get working immediately.[74]
[*]These are available here: “Legislative Reports” (Michigan Department of Licensing and Regulatory Affairs, 2023), https://perma.cc
Most people agree that governments should properly balance the tradeoffs involved with restricting who can work legally in an effort to reduce the risks of harm faced by the public. The problem is that the benefits of licensing laws rarely outweigh their costs. In other words, licensing mandates often needlessly block people from legal employment and only rarely provide a net benefit to the public. That should change.
There are four key reforms that would balance protections for the public and the right to legal employment. Michigan has already accomplished one of those four reforms in 2018 when it passed a law that prohibits local municipalities and governments from creating their own licensing requirements. The other three key reforms are described below.
There are about 180 occupational licenses on Michigan’s books. Many of them also exist in other states, but some are unique to Michigan. Some entail reasonable requirements and ensure a basic level of proficiency for licensed workers. But others require training and costs that far exceed what workers face in other states.
The state should establish a “sunrise” and “sunset” review process. A sunrise review would analyze newly proposed occupational licenses, while a sunset process would require periodic reviews of existing ones. An independent board should assess these regulations, considering their stringency and likelihood of improving public health and safety. A committee in 2012 analyzed occupational licensing and called for eliminating licenses covering two dozen jobs. It also called for loosening rules for many other occupations.[75] The Legislature adopted some of these recommendations, but a review of this kind should be a regular event.
A 2020 Mackinac Center report proposed a process for how these reviews could work, including what factors to evaluate when determining whether a license was necessary and effective.[76] Listed below are some key factors these reviews should consider.
Complaints about qualified worker shortages are common in many industries. Media regularly report about teacher shortages, a deficit of road builders and the need for more construction workers. The lack of doctors, nurses and dentists reportedly drives up medical costs.
This is Economics 101 — supply and demand. A major restriction on the supply of medical professionals is the state’s licensing regime, which makes it needlessly more difficult for professionals from other states to find work in Michigan. Universal reciprocity of all occupational licenses, certifications and training would help. If the state would automatically recognize licenses approved by other states, businesses could hire more workers, medical providers could start serving the public immediately and employment opportunities in Michigan would grow.
Nearly one million jobs in Michigan require a license or certification, and most of these jobs were out of reach for anyone with a misdemeanor or felony on their record. No one should be forced to hire someone with a criminal record, but employers who want to take a chance on individuals trying to better themselves should have the option to employ them. A bill package in Michigan on this issue passed in 2019, but many restrictions remain. Lawmakers should review every law that restricts people with a criminal background from obtaining a license, and only prohibit a license for people who committed serious crimes that are directly related to the occupation they want to go into or that present a meaningful risk to public safety.
Many people often assume that if someone is licensed it automatically means that person is more highly skilled and practicing more safely. Policymakers or state licensing departments, however, only rarely investigate whether this assumption is true. In fact, there are many reasons to suspect that licensing requirements do not per se improve the quality or safety of a service or product.
Here’s just one example: A few years ago, two Detroit funeral homes made national news for improperly storing the bodies of deceased infants and violating a host of other laws. In one funeral home, 63 dead infants were found and the parlor was billing the government for burials that never happened. In the other, “deplorable, unsanitary conditions” and a mummified fetus stored in the ceiling tiles was found.[77]
None of the reports about this tragedy drew attention to the fact that these were properly licensed funeral homes. There was no mention of the overly broad regulations of Michigan funeral homes or that other states do not require this license.[78] Unmentioned too was the research that suggests licensing funeral homes needlessly raises costs for consumers.[79] Nevertheless, the operators of these funeral homes apparently passed all the regulatory hurdles, met the education requirements and paid their fees. But the licensing requirement and the state’s regulatory regime did not prevent or even detect these blatant abuses.[80]
This is just one example, of course, but regulatory rules are intended to protect the public. If they fail on that account, what else justifies their use? Too often, occupational licensing rules amount to mere obstacles that make it more difficult for people to find work. They are not often designed and managed to focus specifically on improving public health and safety.
If licensing laws were truly dedicated to protecting the public and consumers, we would expect to find similar rules for similar occupations. Laws among the 50 states would be similar. Instead, we find a hodgepodge of varying licensing rules and regulations that exist across industries, occupations and state lines.
Michigan should reform its licensing regime and remove needless barriers to work for residents. The state should only mandate licenses when there is a demonstrable and direct connection to protecting consumers. State policymakers have already passed several key reforms that will make it easier for people to find work, but more must be done. They should continue these efforts to focus regulatory rules on protecting public health, regularly review the laws, and avoid adopting new licenses that needlessly raise costs for consumers and discourage Michigan residents eager for work.
1 Morris M. Kleiner, “The influence of occupational licensing and regulation” (IZA World of Labor, October 2017), https://perma.cc
2 Morris M. Kleiner, “A Welfare Analysis of Occupational Licensing in U.S. States” (National Bureau of Economic Research, October 2019), https://perma.cc
3 Janna E. Johnson and Morris M. Kleiner, “Is Occupational Licensing a Barrier to Interstate Migration” (American Economic Journal: Economic Policy, vol. 12, no. 3, August 2020), https://perma.cc
4 Morris M. Kleiner and Evgeny S. Vorotnikov, “At What Cost?:State and National Estimates of the Economic Costs of Occupational Licensing” (Institute for Justice, November 2018), 18, https://perma.cc
5 Chiara Farranato et al., “Consumer Protection in an Online World: An Analysis of Occupational Licensing” (National Bureau of Economic Research, January 2020), https://perma.cc
6 Kyle Sweetland and Dick M. Carpenter II, “Raising Barriers, Not Quality: Occupational Licensing Fails to Improve Services” (Institute for Justice, October 2022), https://perma.cc
7 Mindy Menjou, Michael Bednarczuk and Amy Hunter, “Beauty School Debt and Drop-Outs: How State Cosmetology Licensing Fails Aspiring Beauty Workers” (Institute for Justice, July 2021), https://perma.cc
8 Kathy Sanchez, Elyse Smith Pohl and Lisa Knepper, “Too Many Licenses?: Government ‘Sunrise’ Reviews Cast Doubt on Barriers to Work” (Institute for Justice, February 2022), https://perma.cc
9 “Occupational Licensing: A Framework For Policymakers” (The White House, July 2015), https://perma.cc
10 “Dangerous Jobs” (Compensation and Working Conditions, Bureau of Labor Statistics, Summer 1997), https://perma.cc
11 Morris M. Kleiner and Kyoung Won Park, "Life, limbs, and licensing: occupational regulation, wages, and workplace safety of electricians, 1992–2007," (Monthly Labor Review, Bureau of Labor Statistics, January 2014), https://perma.cc
12 “Where Can Nurse Practitioners Work Without Physician Supervision?” (Simmons University, April 28, 2021), https://perma.cc
13 Morris M. Kleiner et al., “Relaxing Occupational Licensing Requirements: Analyzing Wages and Prices for Medical Service” (The Journal of Law and Economics, vol. 59, no. 2, May 2016), https://perma.cc
14 Shishir Shakya and Alicia Plemmons, “Does Scope of Practice Affect Mobility of Nurse Practitioners Serving Medicare Beneficiaries?” (Journal of Labor Research, vol. 41, Nov. 15, 2020), https://perma.cc
15 Moiz Bhai and David T. Mitchell, “The Effect of Occupational Licensing Reform for Nurse Practitioners on Children’s Health” (Southern Economic Journal, July 3, 2022), https://perma.cc
16 “License Types & Active Counts” (Michigan Department of Licensing and Regulatory Affairs, Bureau of Professional Licensing, May 17, 2023), https://perma.cc
17 “Economy at a Glance: Michigan” (U.S. Bureau of Labor Statistics, 2023), https://perma.cc
18 Based on data available at mischooldata.org.
19 Elizabeth Raczkowski, “Occupational Licensing in Michigan” (Michigan Senate Fiscal Agency, Summer 2019), https://perma.cc
20 Noah Trudeau and Edward Timmons, “2023 State Occupational Licensing Index,” (Archbridge Institute, March 2023), 11, https://perma.cc
21 Patrick McLaughlin et al., “The State of Occupational Licensure in Michigan” (Mercatus Center, Feb. 28, 2018), https://perma.cc
22 Patrick McLaughlin et al., “The State of Occupational Licensure in Michigan” (Mercatus Center, Feb. 28, 2018), https://perma.cc
23 “Michigan’s Occupational Licensing Requirements” (Mackinac Center for Public Policy, 2023), https://perma.cc
24 For more about this, see: Jarrett Skorup, “This Isn’t Working: How Michigan’s Licensing Laws Hurt Workers and Consumers” (Mackinac Center for Public Policy, March 15, 2017), 8-9, https://perma.cc
25 George J. Stigler, “The Theory of Economic Regulation” (Bell Journal of Economics and Management Science, vol. 2 (Spring), 1971), https://perma.cc
26 Tom Gantert, “1,200 Hours To Be a Lawyer, But 2,000 To Be a Barber” (Michigan Capitol Confidential, Mackinac Center for Public Policy, April 16, 2012), https://perma.cc
27 Jarrett Skorup, “Michigan Considering Excessive Hunting and Fishing Regulations” (Mackinac Center for Public Policy, March 13, 2020), https://perma.cc
28 Jeff Stoutenburg and Paul Holland, “Repeal Licensure of Dieticians & Nutritionists: House Bill 4688” (Michigan House Fiscal Agency, Oct. 14, 2013), https://perma.cc
29 Jarrett Skorup, “Michigan Should Not Bring Back Dietitian and Nutritionist Licensing” (Mackinac Center for Public Policy, May 10, 2022), https://perma.cc
30 Jarrett Skorup, “MichiganVotes: Legislation Would Eliminate Licensing Mandate on Dieticians, Nutritionists” (Michigan Capitol Confidential, Mackinac Center for Public Policy, June 1, 2013), https://perma.cc
31 Susan Stutzky and Marcus Coffin, “Mortuary Science Licensure Requirements: House Bill 4437 as enacted” (Michigan House Fiscal Agency, April 2, 2021), https://perma.cc
32 Jarrett Skorup, “No Evidence Michigan License for Funeral Homes is Effective” (Mackinac Center for Public Policy, May 15, 2020), https://perma.cc
33 Jarrett Skorup, “You Shouldn’t Need a License to Work as a Property Manager” (Mackinac Center for Public Policy, July 16, 2021), https://perma.cc
34 Jarrett Skorup, “National Groups Push Music Therapist Licensing – Which Benefits Themselves” (Mackinac Center for Public Policy, Sept. 5, 2019), https://perma.cc
35 Madeline Petlzer, “Possible Fire Sprinkler License Would Be Nation’s Most Restrictive” (Michigan Capitol Confidential, Mackinac Center for Public Policy, July 15, 2019), https://perma.cc
36 Jarrett Skorup, “Michigan Food Delivery Drivers Don’t Need New Government Mandates” (Mackinac Center for Public Policy, Feb. 11, 2022), https://perma.cc
37 Jarrett Skorup, “Michigan Unwisely Moving to Add New Licensing Requirements on Solar Panel Installers” (Mackinac Center for Public Policy, June 4, 2021), https://perma.cc
38 Edward Timmons and Jarrett Skorup, “State licensing should only be a last resort” (The Detroit News, June 2, 2018), https://perma.cc
39 “2018 Senate Bill 826: Impose licensure on “naturopathic physicians” (MichiganVotes.org, Mackinac Center for Public Policy, 2023), https://perma.cc
40 “2015 House Bill 4598: Impose licensure on midwives” (MichiganVotes.org, Mackinac Center for Public Policy, 2023), https://perma.cc
41 Madeline Peltzer, “New Licensure Mandate And Fees Make It Harder To Be A Midwife” (Michigan Capitol Confidential, Mackinac Center for Public Policy, July 12, 2019), https://perma.cc
42 Scott McClallen, “Bill aims to add Michigan to Nurse Licensure Compact” (The Center Square, Feb. 16, 2021), https://perma.cc
43 Jarrett Skorup, “Three Reforms to Bring Down Michigan Health Care Costs” (Michigan Capitol Confidential, Mackinac Center for Public Policy, May 18, 2016), https://perma.cc
44 Ted Roelofs, “Giving Michigan nurses more authority to prescribe drugs and treat patients” (Bridge Michigan, Oct. 8, 2015), https://perma.cc
45 Jarrett Skorup and Lindsay B. Killen, “Michigan Should Permanently Loosen Restrictions on Medical Scope of Practice, Not Reinstate Them” (Mackinac Center for Public Policy, Aug. 3, 2020), https://perma.cc
46 Evan Carter, “Need A License To Shampoo Hair For Pay? Michigan Says ‘Yes’” (Michigan Capitol Confidential, Mackinac Center for Public Policy, July 25, 2017), https://perma.cc
47 Derek Draplin, “Good With His Hands, But Sidelined By Massage License Requirement” (Michigan Capitol Confidential, Mackinac Center for Public Policy, March 21, 2017), https://perma.cc
48 Jarrett Skorup, “Vet Saves Dog's Life, Family is Happy – State Sanctions Him” (Michigan Capitol Confidential, Mackinac Center for Public Policy, July 14, 2016), https://perma.cc
49 Jarrett Skorup, “Past Mistakes Haunt Builder Trying to Find Work” (Michigan Capitol Confidential, Mackinac Center for Public Policy, Dec. 22, 2017), https://perma.cc
50 Evan Carter, “State Law May Drive Job-Seeking Michigan Woman To Move Elsewhere” (Michigan Capitol Confidential, Mackinac Center for Public Policy, April 13, 2018), https://perma.cc
51 Evan Carter, “State Licensure Mandate Ensnarls Another Hair Braider” (Michigan Capitol Confidential, Mackinac Center for Public Policy, Aug. 4, 2017), https://perma.cc
52 Keely Lovern, “Holland hair braider fighting to change license laws in the State of Michigan” (WZZM, March 23, 2022), https://perma.cc
53 “Frequently Asked Questions – General Licensing Issues” (Michigan Department of Licensing and Regulatory Affairs, Sept. 24, 2010), https://perma.cc
54 MCL § 339.2403(f).
55 Jarrett Skorup, “Superintendent Earns Praise Painting School – Which Would Be Illegal If He Were Paid” (Mackinac Center for Public Policy, Aug. 16, 2018), https://perma.cc
56 Jarrett Skorup, “Want More School Librarians in Michigan? Reform State Licensing Law” (Mackinac Center for Public Policy, Aug. 15, 2019), https://perma.cc
57 “Farmers Market FAQ” (Michigan Department of Agriculture & Rural Development, 2023), https://perma.cc
58 “Explanation of Nursery License Types” (Michigan Department of Agriculture and Rural Development, Aug. 8, 2022), https://perma.cc
59 “Michigan’s Occupational Licensing Requirements” (Mackinac Center for Public Policy, 2023), https://perma.cc
60 “Learn to Fly” (University of Michigan Flyers), https://perma.cc
61 “1500 Hour Rule” (ATP, 2023), https://perma.cc/7YWK-KMBN; Evan Carter, “Need A License To Shampoo Hair For Pay? Michigan Says ‘Yes’” (Michigan Capitol Confidential, Mackinac Center for Public Policy, July 25, 2017), https://perma.cc
62 “Basic Training Curriculum and Training Objectives” (Michigan Commission on Law Enforcement Standards, 2022), https://perma.cc
63 For more information about these specific bills, see the following descriptions provided by MichiganVotes.org: “2013 House Bill 4684: Repeal auctioneer registration mandate,” https://www.michiganvotes.org
64 For more information about these specific bills, see the following descriptions provided by MichiganVotes.org: “2019 Senate Bill 434: Authorize rules for cosmetology ‘mobile salons’,” https://www.michiganvotes.org
65 Rick Yuille, Patrick Morris and Ben Gielczyk, “Local Government Occupational Licensing Act” (Michigan House Fiscal Agency, Dec. 28, 2018), https://perma.cc
66 Jamie A. Hope, “Lucky 8-Ball Says: Signs Point To Legal Trouble for Local Bans Of Fortune Tellers” (Michigan Capitol Confidential, Mackinac Center for Public Policy, April 22, 2022), https://perma.cc
67 Lansing Code of Ordinances, “Chapter 805 – Auctions” (City of Lansing, April 4, 2023), https://perma.cc
68 “Apply for a Snowplow Business License” (City of Grand Rapids, 2023), https://perma.cc
69 Jarrett Skorup, “Reduce licensing, get Detroit booming again” (The Detroit News, March 30, 2017), https://perma.cc
70 Jamie A. Hope, “Detroit Repeals Some Burdensome Business And Occupational License Mandates” (Michigan Capitol Confidential, Mackinac Center for Public Policy, March 16, 2022), https://perma.cc
71 Susan Stutzky and Marcus Coffin, “‘Good Moral Character’ Requirements” (Michigan House Fiscal Agency, Jan. 27, 2021), https://perma.cc
72 Jamie A. Hope, “Did The Crime, Served The Time — And Now He Can Make A Living” (Michigan Capitol Confidential, Mackinac Center for Public Policy, March 26, 2022), https://perma.cc
73 “Good Moral Character Report Fiscal Year – 2021” (Michigan Department of Licensing and Regulatory Affairs, Nov. 30, 2021), https://perma.cc
74 Tyler VanHuyse and Joe Carrasco, Jr., “Licensin [sic] Req.; Veteran Exemptions” (Michigan Senate Fiscal Agency, Aug. 17, 2022), https://perma.cc
75 “Recommendations Of The Office Of Regulatory Reinvention Regarding Occupational Licensing” (Michigan Office of Regulatory Reinvention, Feb. 17, 2012), https://perma.cc
76 Jarrett Skorup and Thomas Hemphill, “How To Analyze Occupational Licensing Laws” (Mackinac Center for Public Policy, 2020), https://perma.cc
77 Fiona Kelliher, “Detroit fetal remains scandal: What we know” (Detroit Free Press, Oct. 22, 2018), https://perma.cc
78 Parker Thayer, “Why Can Funeral Directors Only Manage One Home Per County?” (Michigan Capitol Confidential, Mackinac Center for Public Policy, June 17, 2020), https://perma.cc
79 Brandon Pizzola and Alexander Tabarrok, “Occupational licensing causes a wage premium: Evidence from a natural experiment in Colorado’s funeral services industry” (International Review of Law and Economics, vol. 50, June 2017), https://perma.cc
80 Hasan Dudar, “Officials: Mold-covered bodies found at Detroit funeral home” (Detroit Free Press, April 25, 2018), https://perma.cc